Hip Dysplasia Research - Latest Findings
Hip Dysplasia Research - Latest FindingsHip Dysplasia Research - Latest FindingsHip Dysplasia Research - Latest FindingsHip Dysplasia Research - Latest Findings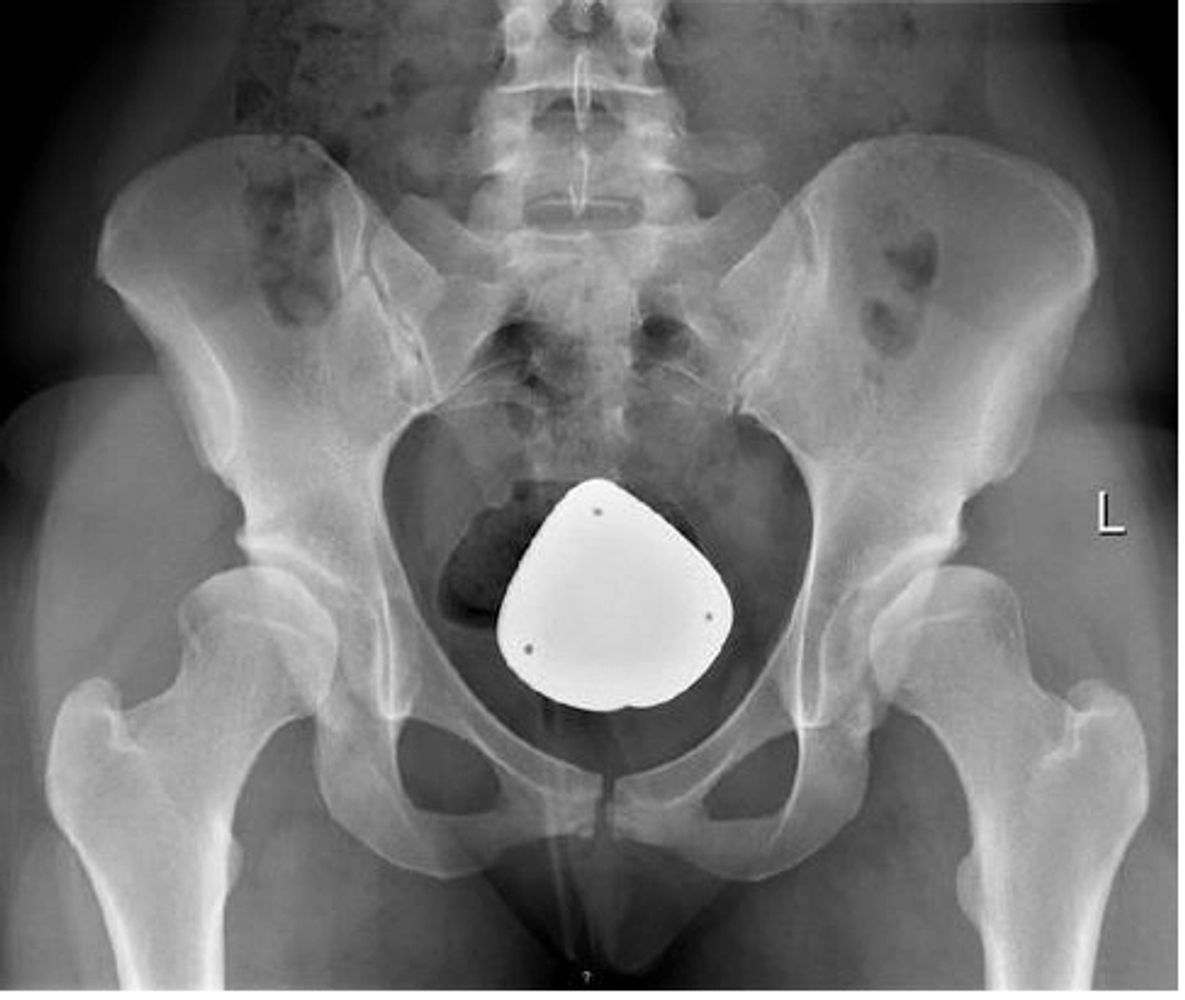

Hipdysplasiaphysio.com was established by Holly Soper-Doyle, a specialist musculoskeletal physiotherapist at The Royal National Orthopaedic Hospital (Stanmore) and the owner of Integrum Physiotherapy in North London. Holly recognized a significant gap in the resources available for the rehabilitation of hip dysplasia, covering both conservative management and pre & post-operative care, and aimed to create a valuable resource for patients and physiotherapists alike. She actively mentors hip dysplasia patients around the world via social media and, after noticing various issues with rehabilitation practices, decided to provide an evidence-based educational website featuring essential rehabilitation guidelines. This website is dedicated to enhancing understanding of hip dysplasia and emphasizes the importance of proper physiotherapy both pre and post-operatively, along with the latest research, including insights on procedures like Periacetabular Osteotomy.

Hip dysplasia is a condition characterized by the hip joint's socket (acetabulum) being too shallow. This condition may be present from birth or can develop during growth phases. Hip dysplasia is more prevalent in women, with a ratio of 8:2 compared to men, and it is a well-known precursor to early onset osteoarthritis.
There is evidence suggesting genetic links to hip dysplasia, as individuals are 12 times more likely to develop it if there is a family history. Several predisposing risk factors include the position in the womb, breech birth, female gender, and certain carrying positions as an infant. These factors can contribute to increased ligament laxity and poor bony congruency.
Patients with hip dysplasia often begin to experience symptoms in their late teens, 20s, or 30s. Due to the shallow hip socket, increased shearing forces act on the joint, leading to damage around the front edge of the socket over time, resulting in pain.
One of the initial signs of hip dysplasia is often pain due to a tear in the labrum, which is a piece of cartilage that provides negative suction to the joint. Symptoms may include pain in the anterior hip joint, catching, painful clicking, and a sensation of the joint giving way.
Once pain begins, it indicates that the joint can no longer withstand the resultant increased shearing forces caused by the shallow socket. Consequently, the joint may start to degenerate, with damage occurring to the articular cartilage, which is the gliding surface of the joint, leading to the gradual development of osteoarthritis.
If hip dysplasia is left undiagnosed and/or untreated, the joint can degenerate to the point of bone-on-bone contact, necessitating surgical interventions such as a Periacetabular Osteotomy or hip replacement. In addition to surgical options, physiotherapy can provide critical physiotherapy advice and rehabilitation guidelines to support recovery and maintain joint function.
Hip dysplasia can be diagnosed using a plain x-ray of the pelvis. The medical professional should examine the lateral centre edge angle of each hip socket, which indicates whether there is uncovering of the femoral head. A dysplastic hip is characterized by a lateral centre edge angle of less than 20 degrees, while borderline dysplasia is indicated by angles between 20-25 degrees. Normal values range from 25-40 degrees. To further assess the integrity of the joint and surrounding structures and to identify any resultant damage, CT and/or MRI can be employed. For a clinical diagnosis of a labral tear, an MR Arthrogram is necessary, as it provides more sensitivity and specificity in detecting labral tears compared to a standard MRI. This procedure includes injecting dye into the hip joint followed by an MRI. In cases of severe hip dysplasia, a Periacetabular Osteotomy may be considered, along with appropriate physiotherapy advice and rehabilitation guidelines to support recovery.

Hip dysplasia is a condition that can significantly impact mobility, often requiring surgical interventions such as Periacetabular Osteotomy. Following surgery, effective physiotherapy plays a crucial role in recovery. It's essential to adhere to physiotherapy advice and rehabilitation guidelines to ensure the best outcomes during the rehabilitation process.
Integrum Physiotherapy is a north London based Physiotherapy service provided by Holly Soper-Doyle, specializing in conditions such as hip dysplasia and offering guidance on rehabilitation guidelines following procedures like Periacetabular Osteotomy. If you wish to book a home visit with Holly for personalized physiotherapy advice, pleas
Integrum Physiotherapy is a north London based Physiotherapy service provided by Holly Soper-Doyle, specializing in conditions such as hip dysplasia and offering guidance on rehabilitation guidelines following procedures like Periacetabular Osteotomy. If you wish to book a home visit with Holly for personalized physiotherapy advice, please contact her using the options below: Email: integrumphysio@protonmail.com Website: www.integrumphysiotherapy.co.uk Telephone: 07863125719

This article highlights important research into hip dysplasia, focusing on both surgical options like Periacetabular Osteotomy and conservative management strategies. It also emphasizes the role of physiotherapy, providing valuable physiotherapy advice and rehabilitation guidelines for effective recovery.

Having qualified as a Physiotherapist from Brunel University in 2007, Holly has over fifteen years of extensive clinical experience after working in a variety of different specialities, including multiple NHS trusts, Headley Court (the Ministry of Defence rehabilitation centre), and Premiership sports teams like Chelsea and QPR. In 2018, Holly was appointed as an Honorary Clinical Lecturer at UCL, where she teaches on a master's program in Rehabilitation and also earned a Postgraduate Diploma with distinction in Veterinary Physiotherapy.
Holly worked part-time at the Royal National Orthopaedic Hospital (Stanmore) as a specialist hip physiotherapist, enjoying close links with some of the country's leading consultants. She has recently transitioned to work as an Advanced Practice Physiotherapist in the Young Adult Hip Team at Addenbrooke's Hospital in Cambridge. Additionally, she owns her own business, Integrum Physiotherapy, located in North London, where she provides physiotherapy advice to clients in person and via virtual consultations worldwide.
Holly has co-authored a chapter on hip dysplasia in the book 'Hip and Knee Pain Disorders' and has been involved in research projects focusing on hip dysplasia, gluteal tendinopathy, and femoro-acetabular impingement. She also co-wrote a leaflet on hip dysplasia, which is now utilized globally.
In addition to her extensive clinical experience, Holly has personal experience living with developmental dysplasia of the hip (DDH). Diagnosed in 2011 at the age of 25 with bilateral hip dysplasia, she underwent a left Periacetabular Osteotomy in late 2011. Due to significant blood loss during the operation, the rotation was insufficient, and she subsequently required a salvage procedure in 2013, which included a combined Shelf-acetabuloplasty and arthroscopy with labral repair. Her right hip is severely dysplastic with a large labral tear, which she has managed consistently with conservative management.
Holly is passionate about helping people manage DDH and rehabilitate to the best of their ability. This website is dedicated to providing valuable information about hip dysplasia and highlighting the correct rehabilitation guidelines.
Please contact us directly with any questions or comments regarding hip dysplasia, Periacetabular Osteotomy, or for physiotherapy advice and rehabilitation guidelines.